Trigger Warning: This birth story discusses trauma, topics discussed include forceps delivery, emergency theatre and postpartum haemorrhage, and NICU stay. If you are seeking support for your birth trauma, we have downloadable resources here or join one of our free Peer2Peer Support programs.
As a first time mum, I didn’t quite know what to expect during birth. I had taken classes, and read plenty of books, but I couldn’t really imagine what it would be like. All I could picture was, regardless of the type of birth, the moment that I pulled my baby to my chest for the first time. That was what birth looked like for me.
I never got to experience that moment.
I had hyperemesis gravidarum throughout my pregnancy, but otherwise myself and baby were well. I was fortunate enough to get into a ‘continuity of care’ model and had the same midwife throughout my pregnancy (highly recommend!). When I went past my due date, there was pressure from the hospital to be induced, where I was told my baby would die – and I was so thankful to be able to discuss my options with my midwife. I decided that I would wait until 42 weeks, with daily monitoring at hospital in the meantime. I had an ultrasound at 41+3 to check my placenta, but I wasn’t aware that this included a ‘growth check’. I was told that my baby was too big, and that I needed to have a c-section. With support from my midwife, I declined. That night, I received a call from a doctor telling me I had to go in for a c-section, or my baby would die. I continued to receive calls from the hospital over the next few days, harassing me to book in for a c-section.
At 41+6 weeks, I agreed to be induced – mainly because I was sick of fighting. It was also the day Perth went into a ‘snap lockdown’ – meaning that I wasn’t allowed a support person (my partner) to come into hospital with me. I woke that morning in pain, and vomiting continuously, with hospital staff unsure why – they gave me morphine and promised I’d be induced soon. I spent the next three days in the hospital, on continuous monitoring, my partner anxiously pacing outside, while they told me ‘soon’. Each time, I was relieved – I didn’t want to be induced, and I had only said yes because I felt I was supposed to. But at that point I hadn’t been able to keep food or water down for several days, and I just wanted my partner – it got to the point that I begged them for a c-section, just so I could have him with me again.
On Wednesday morning, they prepped me for a c-section. I sat in the waiting room, vomiting. A staff member came to check on me and asked if I was in labour. I shook my head. They had been monitoring me, and it was only Braxton Hicks they said. She called an obstetrician, who agreed to do a cervical examination – 6cm dilated. Finally on Wednesday afternoon I got to see my midwife and my partner again, and things were happening! I thought this would be the easy part – I had fought my way to not being induced, and now I could just let my body birth. But the hospital staff demanded continuous monitoring – which my midwife was able to push back on for several hours – and suddenly there was a time limit. I wasn’t progressing fast enough, they said. I was fully dilated, but my contractions had stopped. I needed a c-section, they said.
With support from my midwife, I managed to negotiate having an epidural instead. My contractions didn’t return, but my midwife was able to stop them from interfering and let me sleep. In the morning when I woke, she was gone, having been there for 16hrs – and I was back to being at the mercy of hospital staff. They needed to get this baby out, they said. My contractions had returned on their own, and I wanted to try pushing. That wasn’t fast enough – they gave me synthetic hormones to ‘speed things up’. Baby passed meconium. Now, they said – and wheeled me to theatre for a forceps delivery, while my partner waited behind as they prepped me. He stood against the wall, COVID-safe distancing.
I will never know what caused it. Maybe it was all the unwanted intervention beforehand, and all the stress in the lead up – or maybe it was because I went past 42 weeks – or maybe it was the use of forceps. But baby and I were fine beforehand – baby had a strong heartbeat, and I was feeling fit and healthy – and somehow, between the labour room and baby being delivered, she had inhaled meconium. I never knew anything was wrong until they pulled her out of me. But I opened my arms to take her, to hold my baby to my chest, and all these hospital staff had descended on her and taken her awaz. A staff member squeezed my hand and told me, ‘congratulations’ – but I didn’t know what for. Nobody told me what was happening. There were hands on my stomach, and then they were wheeling my baby away. My partner had tears in his eyes, and he was trying so hard not to look scared. And then I had to go, too, and they took me to special care unit, my partner left behind.
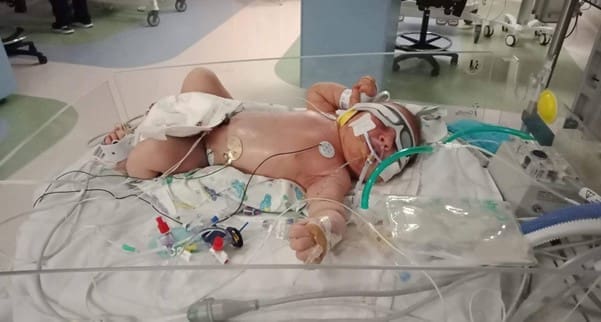
It took hours to know what was happening. I had a haemorrhage, 1.5L, but I felt fine. Things felt unreal. They asked me that night if I wanted to call NICU and ask how my baby was, but I said no. I didn’t understand what was happening, or even felt like I had given birth. COVID restrictions meant my partner couldn’t come see me. And they also meant I couldn’t see my baby. I felt removed from it all. Somebody brought me a picture of her. She was grey and covered in tubes. She looked sick. I thought I would go home without a baby.
The next day, my midwife came to visit me. She was going to try, she said. She would put a letter in of ‘special circumstances’ to allow my partner to come see me, and to allow me to see my daughter. Day two and they wheeled me down to NICU, to see my baby girl. She didn’t feel like mine. She was intubated, and I couldn’t hold her. They said she was doing well, but all I could see were the tubes. All I could focus on was the fact that she was sick, and this guilty feeling like I had somehow caused it. On her cot, were her details – nameless, 4.6kgs.
Day 6 and they extubated her. She could breathe on her own! We got to hold her and named her Noa. Day 8 and I was finally discharged from hospital, but I left her behind. She moved into the special care unit, but now they were concerned about brain damage. Her movements were shaky, and she had gone so long without oxygen – but they couldn’t see anything on the scans. It would be a long road, they said.
Day 13, and we could take our baby home. One of the paediatricians came to say goodbye – and confessed she had no idea how our baby had pulled through. I realised then just how sick she had been – and how close we had come to losing her. We took our baby home. It was the first time we could smile at her, without our masks in the way. But we were back to hospital for regular check-ups, as they monitored her for further signs of brain damage.
At 4 months old, our baby girl was officially discharged from hospital care – with no signs of brain damage.
And now, with baby Noa 18 months old, we are preparing for our second birth. This time, I’m preparing for birth by reading up on hospital policies. I’m learning what I can say no to, and I’m compiling the evidence on it. I have been fortunate to access continuity of care again, I have a student midwife on my team. For this birth, I’m planning on being in control, and not letting anyone ‘scare’ me into doing something that doesn’t feel right. I’m abandoning my ‘good girl’ upbringing and leaning into my badass wisewoman.